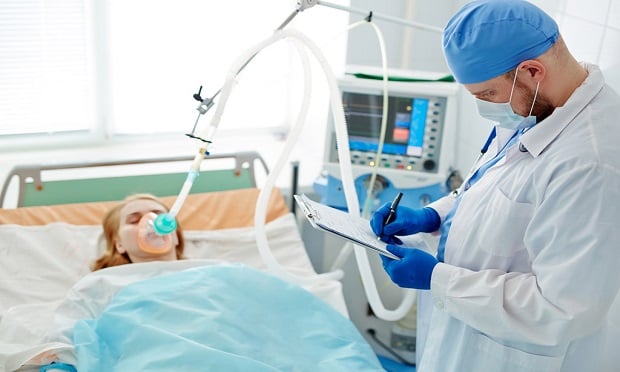
 Many of those stricken with COVID-19 become severely and critically ill, necessitating prolonged hospitalizations in intensive care units (ICUs). (Photo: Shutterstock)
Many of those stricken with COVID-19 become severely and critically ill, necessitating prolonged hospitalizations in intensive care units (ICUs). (Photo: Shutterstock)
The COVID-19 pandemic surprised all of us in January 2020, with its speed of viral infection transmission causing high mortality and morbidity among those afflicted in the United States. This newly formed mutant coronavirus, now known as Severe Acute Respiratory Syndrome Coronavirus 2 or SARS-CoV-2, took the world by storm and many in this country succumbed to severe acute hypoxemic respiratory failures that overwhelmed medical providers, hospitals, communities, and public health organizations in the locales most impacted by the pandemic.
Recommended For You
Want to continue reading?
Become a Free PropertyCasualty360 Digital Reader
Your access to unlimited PropertyCasualty360 content isn’t changing.
Once you are an ALM digital member, you’ll receive:
- Breaking insurance news and analysis, on-site and via our newsletters and custom alerts
- Weekly Insurance Speak podcast featuring exclusive interviews with industry leaders
- Educational webcasts, white papers, and ebooks from industry thought leaders
- Critical converage of the employee benefits and financial advisory markets on our other ALM sites, BenefitsPRO and ThinkAdvisor
Already have an account? Sign In Now
© Touchpoint Markets, All Rights Reserved. Request academic re-use from www.copyright.com. All other uses, submit a request to [email protected]. For more inforrmation visit Asset & Logo Licensing.






