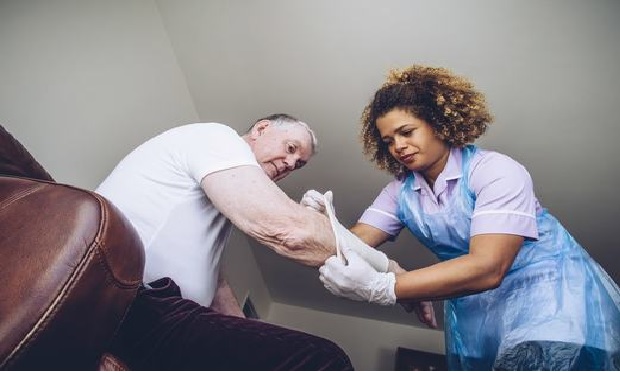
 This patient-centered approach positively affects employee health outcomes and employer spending. In addition to reducing costs for employers by improving outcomes and minimizing indemnity claims, it improves morale by letting injured workers know they are more than just "a case" or a problem to be solved. (Photo: Graham Oliver/Adobe Stock)
This patient-centered approach positively affects employee health outcomes and employer spending. In addition to reducing costs for employers by improving outcomes and minimizing indemnity claims, it improves morale by letting injured workers know they are more than just "a case" or a problem to be solved. (Photo: Graham Oliver/Adobe Stock)
Experience in workers' compensation quickly teaches us that no two companies' situations are the same — every organization and its employees have unique needs, even if they are in the same industry. Despite this, the development of provider networks has traditionally taken a one-size-fits-all approach. As the workers' compensation industry moves toward a patient-centered approach to care, it is time to take a closer look at provider networks and the benefits of a tailored approach.
Patient-first mindset
We are seeing a profound shift in workers' compensation, from a focus on transactions and cost control to patient-centered care. For example, 24/7 triage lines are managed by nurses focused on treating the patient first, communication with injured employees helps them navigate the process, and new technology is being leveraged to spot potential issues in advance and identify solutions. Early detection of these warning signs indicates the need for a course correction within the claims or patient care process, decreasing the likelihood of patient complications or costly, drawn-out claims.
This patient-centered approach positively affects employee health outcomes and employer spending. In addition to reducing costs for employers by improving outcomes and minimizing indemnity claims, it improves morale by letting injured workers know they are more than just "a case" or a problem to be solved.
We are now seeing this patient-first mindset expanding to network solutions. Designing tailored provider networks allows us to move away from the traditional approach of looking at "how many providers can fit in the network" and changes the perspective to "how many providers in this network can deliver the unique outcomes our clients require."
Tailored network solutions
A thoughtfully curated set of providers expedites both care and claims. In contrast to a single group health network, tailored preferred provider networks (PPOs) offer a customized group of network providers based on the unique needs of the organization and its employees.
Tailored PPO networks should be data-based. Information like geographic location and patient injury details, such as the nature and severity of injuries, can be used to identify which types of specialists should be included in the care networks. When used in conjunction with an integrated claims management platform, claims professionals can quickly pivot to meet the needs of injured workers by expanding virtual care services, identifying a more diverse set of medical providers, or speeding up care delivery.
Other benefits of a customized network include:
- The ability to offer injured workers a full spectrum of general and specialty providers, from physical therapists to surgeons to mental health specialists and everything in between
- Greater accessibility to care, whether through virtual or in-person visits
- Improved patient outcomes due to data-driven curated provider networks, leading to swifter treatment and company cost savings
With customized networks, organizations can also take a data-driven approach to measure results and compare them to industry averages, ensuring that the network outperforms them. These data sources include the diagnosis code, time to initial treatment and follow-up treatment, the total cost of the claim, and return-to-work days.
Addressing the whole patient
The best outcomes are achieved by putting patients first, listening to their needs, and advocating for the care they require. Tailored provider networks take a holistic approach to healing the whole person, not just the injury.
Part of this holistic approach is recognizing that injured workers may face social, psychological and biological factors that affect their overall health and recovery. Examples of these situations include:
- Transportation or childcare needed to obtain patient care and attend appointments
- Education or language translation required to understand medication regimens and other aspects of their treatment plan
- Mental health challenges such as anxiety, depression or post-traumatic stress disorder that can arise after a work injury and impact an individual's recovery and ability to return to work
To treat the whole patient, a customized network should include providers who specialize in mental health. Recognizing the importance of mental health and other social concerns allows for prompt and efficient diagnosis and treatment to help accelerate recovery and enable a faster return to work.
Better outcomes at less cost
One might think achieving the best outcomes costs more, but this is not the case. A curated set of providers can support a speedy return to work, even in a modified capacity, offering a financial incentive for employers to adopt this approach.
Customizing a provider network to meet the needs of an individual organization by taking a close look at the company's culture, region, industry and employees is the only way to deliver a superior solution. A holistic, outcomes-based network model provides the best value for employers, insurers, and everyone involved in helping injured workers return to full capacity as soon as possible.
Rhonda Moran is senior vice president, Network Solutions at CorVel. Contact her at Rhonda_moran@corvel.com.
Related:
© Arc, All Rights Reserved. Request academic re-use from www.copyright.com. All other uses, submit a request to TMSalesOperations@arc-network.com. For more information visit Asset & Logo Licensing.